Deborah's 100-Year History Timeline
In its first 100 years of unparalleled care to residents of all twenty-one New Jersey counties, Deborah has healed 2.3 million patients from every state in the US and 87 countries throughout the world.
Deborah® Timeline

Portrait of Founder, Dora Moness Shapiro
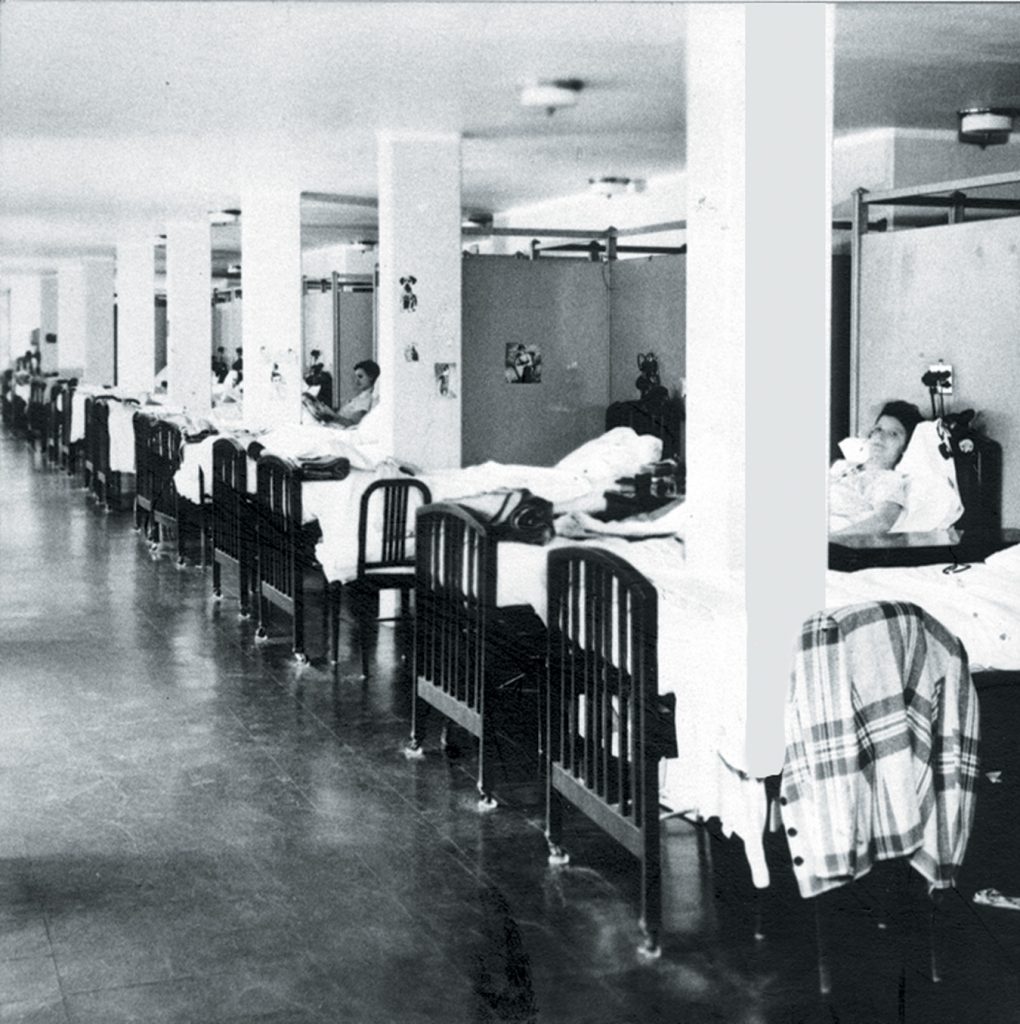
Founder Dora Moness Shapiro first established the hospital as a tuberculosis sanatorium. Back then, the only relief for tuberculosis was rest and fresh air. Determined to make a difference, Shapiro searched for a location outside of New York City that could accommodate the sick and impoverished. Nestled in the heart of Pine Barrens, Shapiro took ownership of an airy cottage well within traveling distance and soon had her first patients.
Former Patient, Clara Falk Franks Organizer of Volunteers and Fundraising Chapters
Clara Falk Franks came to Deborah as a patient in 1934, and remained after she was cured to become a legend in the hospital’s history. For nearly 50 years, Franks raised funds and awareness for Deborah by organizing legions of volunteers into becoming fundraising chapters, and winning support from countless others.
Nobel-Prize Winner and Inventor of TB Drug Visits Deborah
Selman Abraham Waksman, inventor, biochemist and microbiologist whose research into the decomposition of organisms that live in soil enabled the discovery of streptomycin and several other antibiotics, is pictured with Dr. Daniel Rednor, Medical Superintendent, and Clara Franks, Assistant to the President.
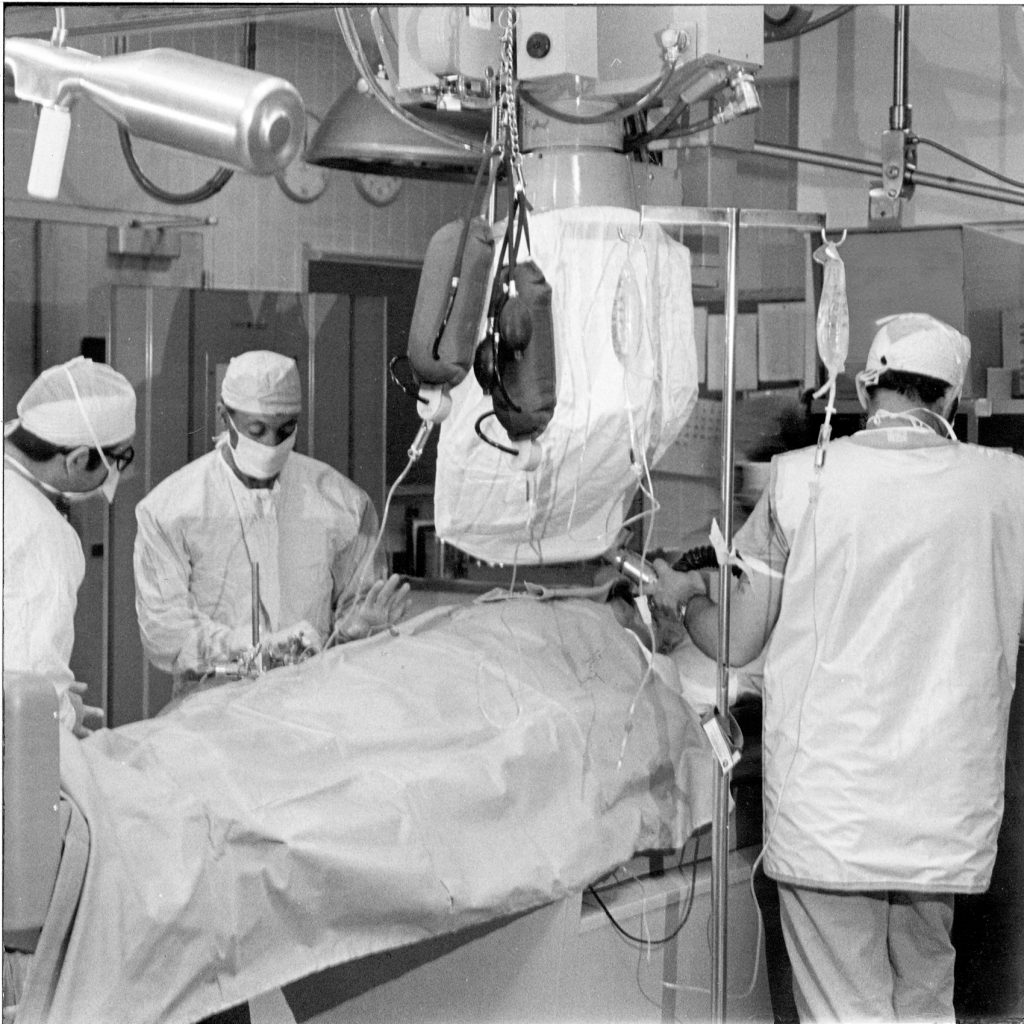
Open Heart Surgery Pioneer
Charles Bailey, M.D., directed cardiovascular surgery at Deborah and his methods were the focus of a 1957 Time magazine article. The first U.S. physician to repair a hole in the wall between the two sides of the heart, Dr. Bailey was born in Wanamassa, N.J., and educated at Rutgers University, Hahnemann Medical College, and the University of Pennsylvania.
Building Expansion Named After Former President Jack Lesser
In 1965, the Lesser Building, named for former Deborah President Jack Lesser, was added to the Main Building, significantly expanding patient care areas. Lesser was named president of the hospital in 1956 after serving as a member of the hospital board for nearly 30 years. During Lesser’s administration the hospital grew from a sanatorium to a treatment and research center for heart and lung diseases.
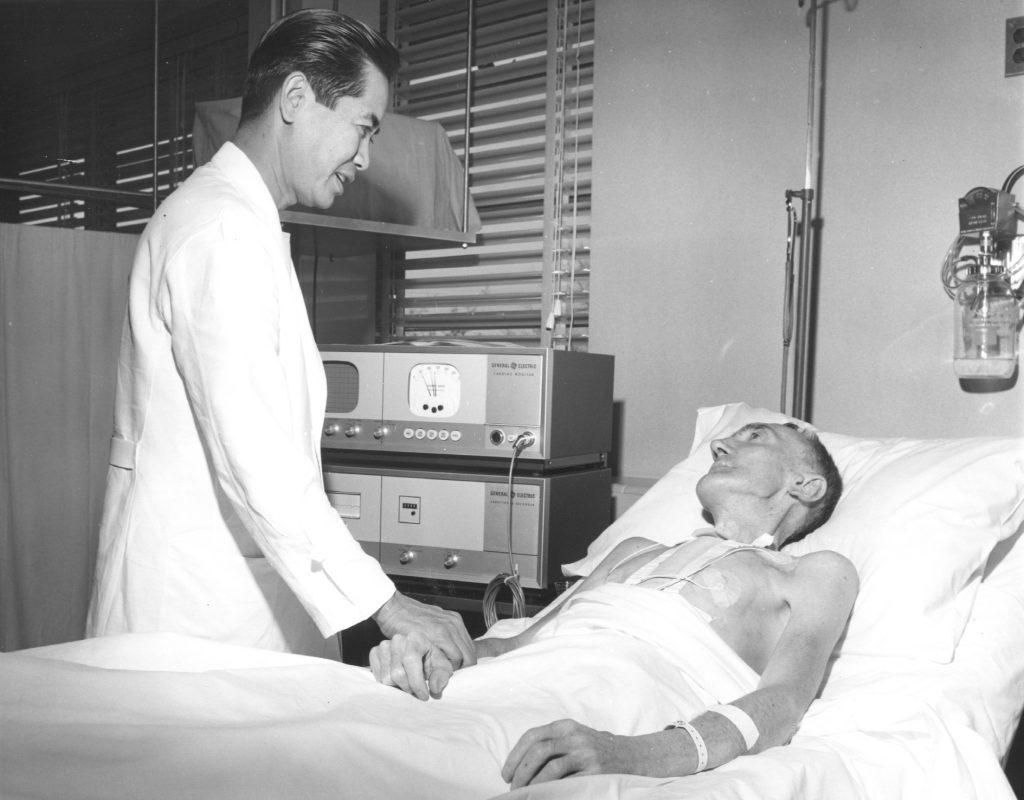
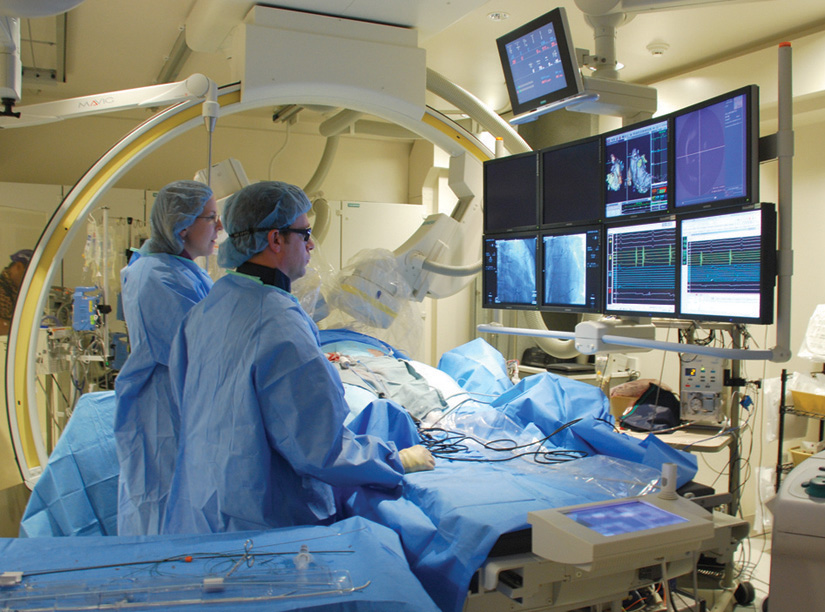
Cardiac Catheterization Labs Added
In 1968 and 1969 new operating suites, cardiac catheterization laboratories and other diagnostic units were added. Cardiac catheterization allows doctors to see how well blood vessels supply blood to the heart. Doctors use contrast dye that they inject into blood vessel through a catheter to create X-ray videos of valves, coronary arteries, and heart chambers.
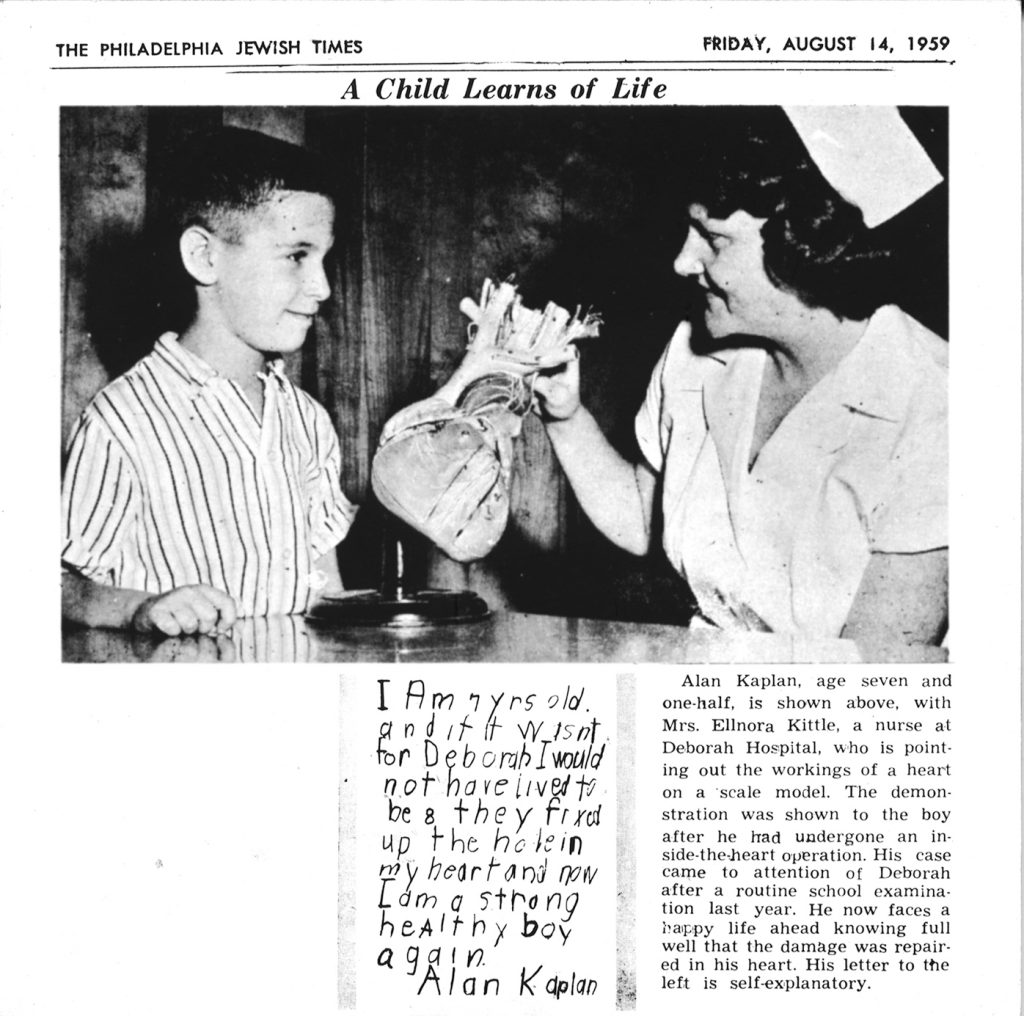
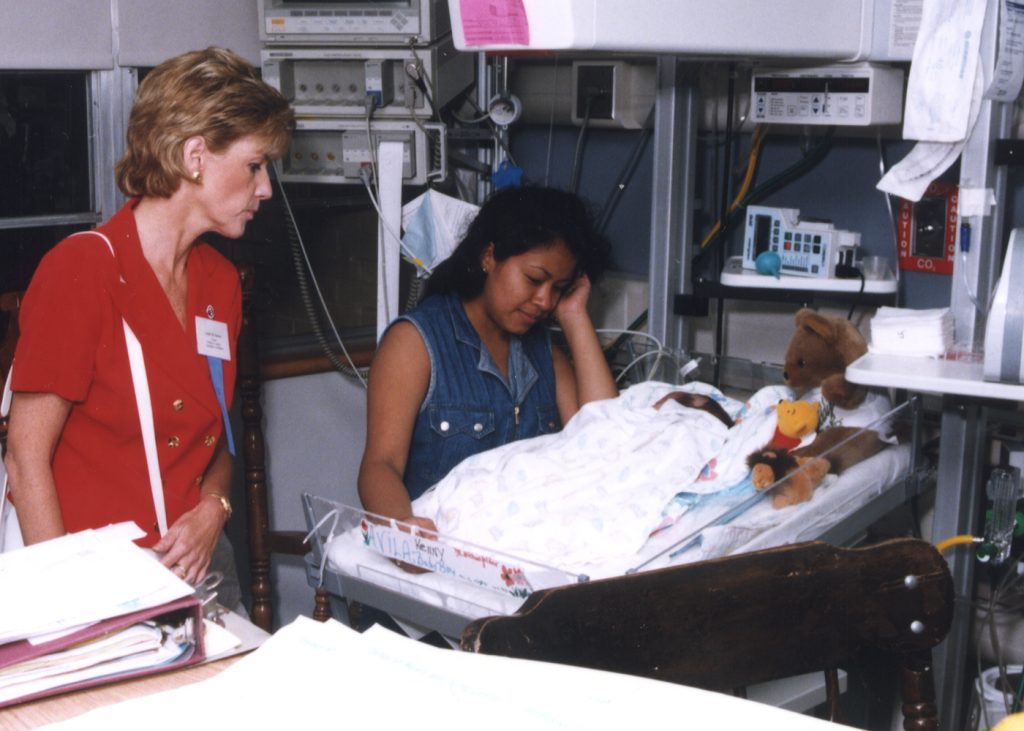
Children of the World Program®
The Children of the World® program began treating pediatric patients with congenital heart defects and other severe medical problems that could not receive advanced heart and lung care in their home countries. Children from more than 80 countries came to Browns Mills for treatment and received care at no cost.
Deborah Hospital Foundation
Incorporated in 1974, Deborah Hospital Foundation is the fundraising entity for Deborah Heart and Lung Center. The Foundation relies annually on the generous support of individuals, corporations, foundations and membership organizations to support the life-saving care provided by the Deborah Heart and Lung Center.
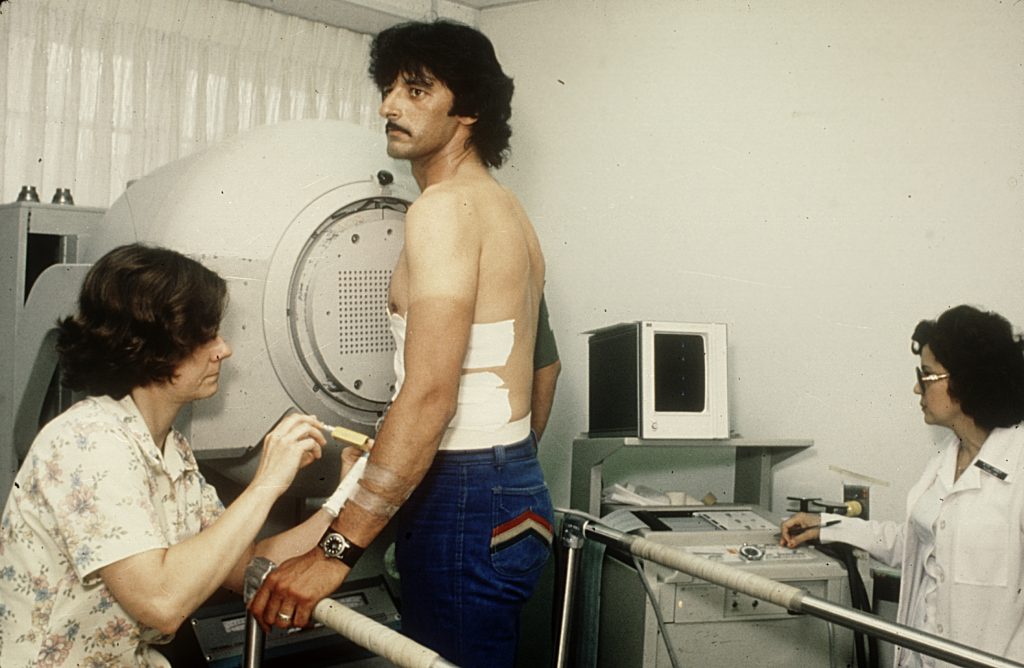
First Nuclear Stress Test Performed at Deborah
On July 13, 1977, Deborah performed its first nuclear stress test. A nuclear stress test uses a small amount of radioactive material (tracer) and an imaging machine to create pictures showing the blood flow to the heart. The test measures blood flow while at rest and during activity, showing areas with poor blood flow or damage in the heart. Today, it is one of the most commonly used tests to diagnose and treat cardiovascular conditions.
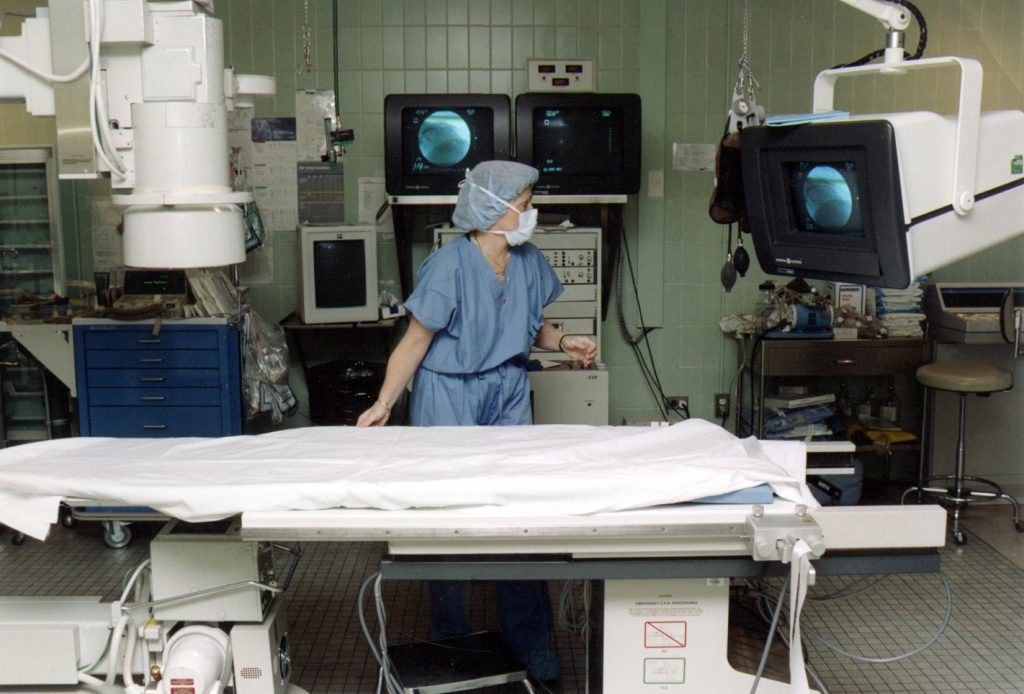
Deborah’s First Balloon Angioplasty
Vladir Maranhao, MD, affectionately known as “Dr. Mara” performed Deborah’s first percutaneous transluminal coronary angioplasty (PTCA) or balloon angioplasty. Dr. Mara also performed Deborah’s first cardiac catheterization in 1959 and spent 28 years at Deborah Heart and Lung Center as a cardiologist, chairman of the department of cardiovascular diseases and later vice president of medical affairs.
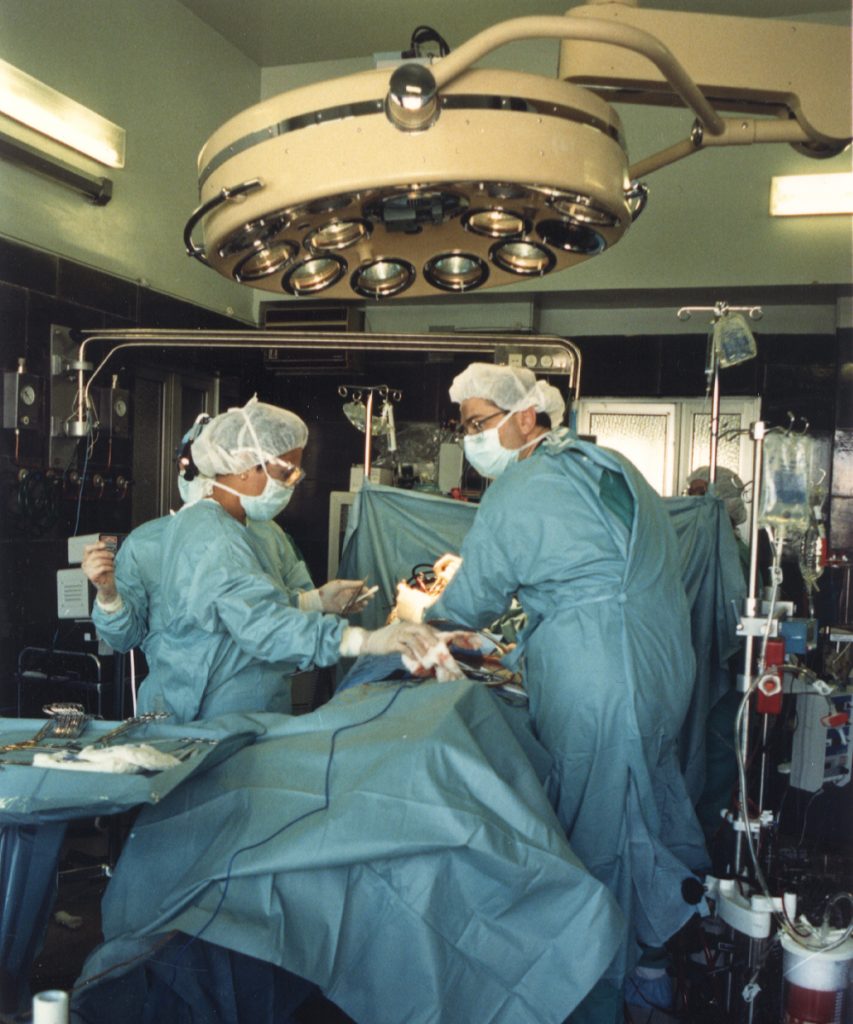
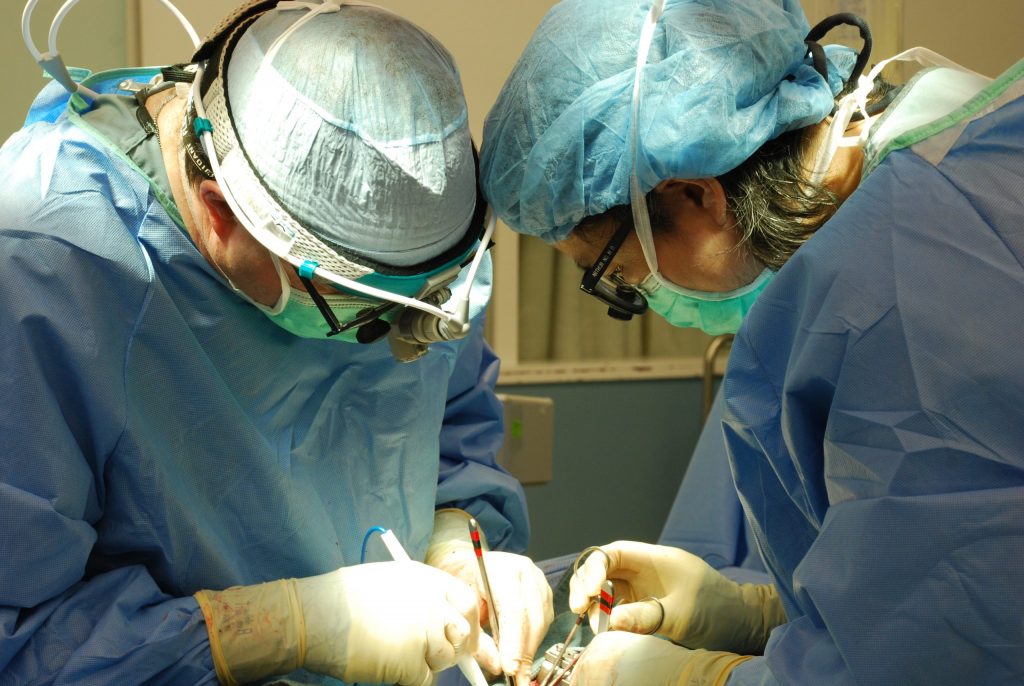
Deborah Travels to Georgian Soviet Socialist Republic to Perform Open Heart Surgery
A 40-member medical, surgical and support team traveled to Georgian Soviet Socialist Republic to perform open heart surgery at a children’s hospital there. The Deborah team performed 19 procedures during their week-long mission, providing aftercare for patients, sharing methods and techniques with their Georgian counterparts.
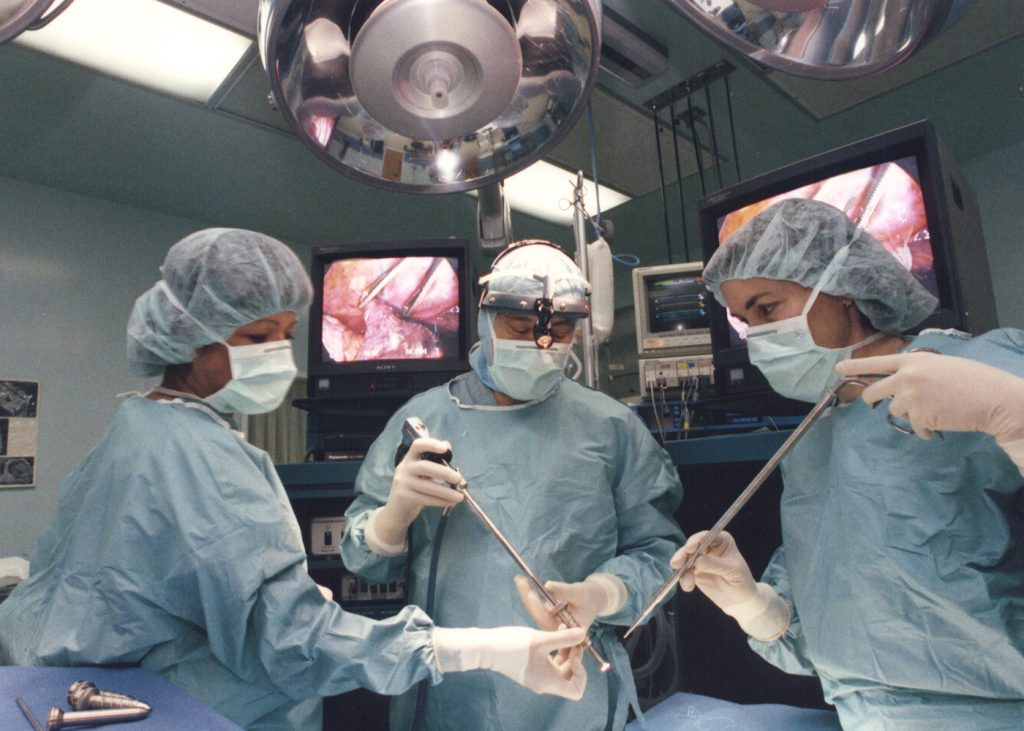
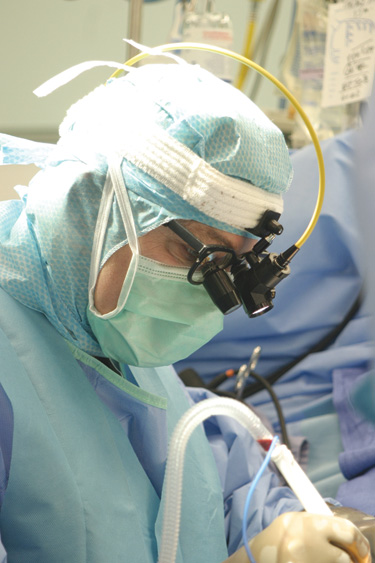
Video-assisted Thoracoscopic Surgery for Lung Biopsy and Tumor Removal Introduced
Video-assisted thoracoscopic surgery (VATS) using fiber optic technology to diagnose and treat problems in the chest become available at Deborah. A tiny camera called a thoracoscope is inserted into the chest through a small incision. This procedure offered patients a less invasive surgical option for lung biopsy and tumor removal and greatly reduced recovery time.
William G. Rohrer Neonatal and Pediatric Cardiac Surgical Unit
In May 1997, Deborah opened the William G. Rohrer Neonatal and Pediatric Cardiac Surgical Unit, which was made possible by a gift from the William G. Rohrer Charitable Foundation. The eight-bed unit, which provides critical pre- and post-operative care to newborns, infants and children, was formally opened and dedicated by Linda Rohrer, Rohrer Foundation trustee, and daughter of the late businessman and philanthropist, who was also a former Deborah Executive Board Member.
Smallest Pacemakers Implanted by Cardiac Electrophysiologist Raffaele Corbisiero, MD
Patients suffering from atrial fibrillation, a form of abnormal heart rhythm obtain groundbreaking care thanks to advances in cardiac electrophysiology. In 2002, Raffaele Corbisiero, MD implanted two of the smallest implantable cardioverter defibrillators (ICD) and pacemakers in the world at Deborah Heart and Lung Center.
Tibetan Monks Perform Hospital Blessing and Good Luck Dance
Eight of the Dalai Lama’s emissary Tibetan monks performed as part of Drepung Gomang Institute Sacred Arts Tour at Deborah in 2011. The monks performed a traditional Tibetan hospital blessing and Good Luck Dance. Deborah was selected as a tour stop because of its history fighting tuberculosis, a prevalent health problem in Southern India where the Monks have a monastery in exile from Tibet.
FDA-approved WATCHMAN™ Device Becomes Available at Deborah
Deborah Heart and Lung Center was among the first in the region to implant the FDA-approved WATCHMAN™ Left Atrial Appendage Closure (LAAC) Implant. This device is a breakthrough for patients with atrial fibrillation as an alternative to long-term warfarin medication therapy. The WATCHMAN™ Implant closes off the left atrial appendage to keep harmful blood clots within the left atrial appendage (LAA) from entering the bloodstream and potentially causing a stroke.
Cleveland Clinic Alliance
Deborah becomes the exclusive Cleveland Clinic Heart, Vascular & Thoracic Institute affiliate in Burlington, Camden, Atlantic, Gloucester, Salem, Cumberland and Cape May counties in New Jersey as well as Bucks and Philadelphia counties in Pennsylvania. This clinical affiliation is part of the strategic plan to continue Deborah’s mission of maintaining the highest standards of quality cardiac care for patients.
Partnership Formed for Graduate Fellowship Training Programs
Deborah Heart and Lung Center announced a partnership with Sidney Kimmel Medical College at Thomas Jefferson University for its graduate fellowship training programs. Fellows work side-by-side with some of the most talented physicians in the country training in advanced cardiovascular techniques and leading-edge clinical trials.
100 Bluetooth Enabled Defibrillators
Deborah becomes the first hospital in the nation to implant 100 Bluetooth enabled defibrillators. The Abbott Gallant™ implantable cardioverter defibrillator (ICD) and cardiac resynchronization therapy defibrillator (CRT-D) devices pair with a smartphone app via Bluetooth, providing remote monitoring for patients with abnormal heart rhythms and heart failure.
Deborah 100 Project
Deborah has embarked on a $100 million capital investment project. Aimed at improving the quality of care, privacy and comfort, consistent with the offerings of a world-class specialty hospital, the project will begin in 2022. This project will result in the addition of three new floors to the main building of the hospital, the renovation of patient rooms, bedside technology, and decentralized work stations for medical staff. There are also plans for a new cardiac catheterization lab, new electrophysiology lab, and a pharmacy cleanroom. Once completed, Deborah’s investment in new infrastructure, with state-of-the art technology, positions Deborah Heart and Lung Center to be a leader in care for the next 100 years.